 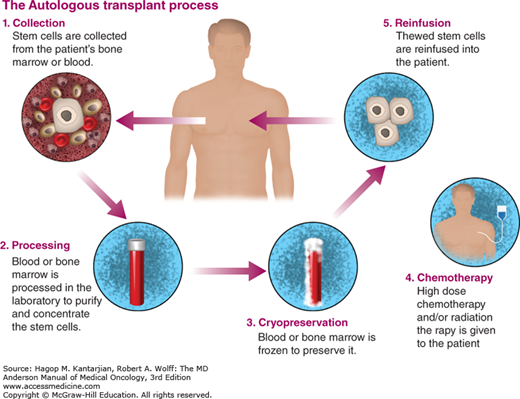 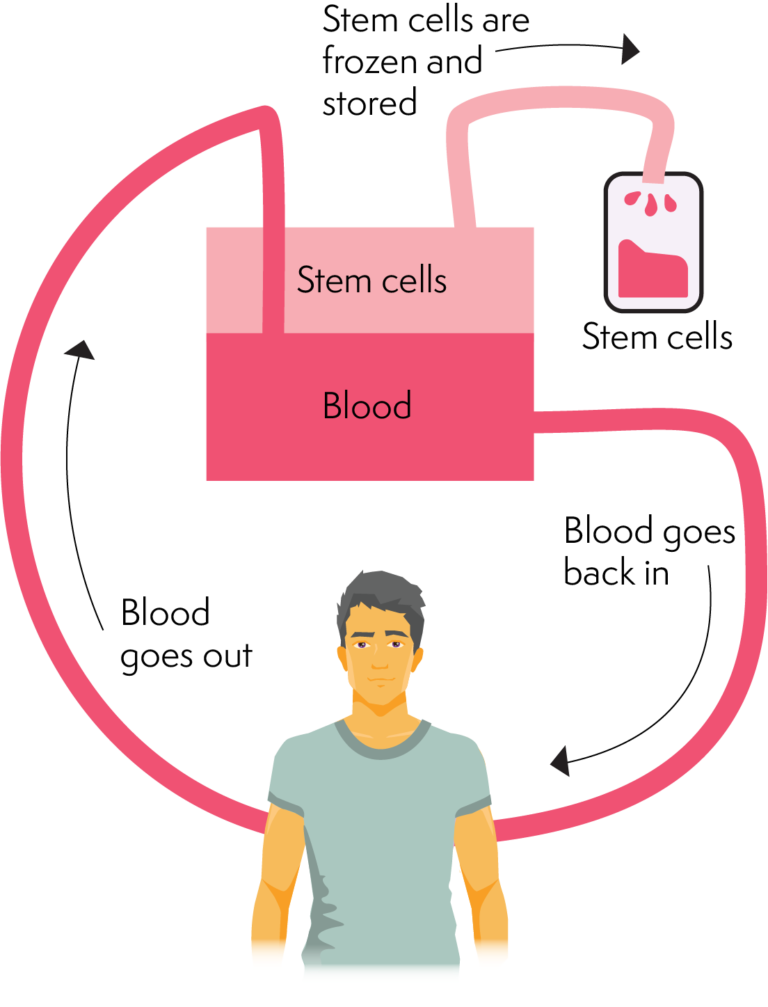
Therefore, it is imperative to evaluate transplant toxicity in an advanced age. Despite these concerns, studies show there is a blatant benefit in survival for transplanted elderly patients, even in analysis adjusted to performance status, comorbidities, and disease stage and after the introduction of novel agents for induction chemotherapy. Īging determines a progressive deterioration of physiological reserves and endurance that may increase morbidity and mortality, jeopardizing the effectiveness of ASCT as part of treatment options in MM. Some studies suggest that age at the time of transplant does not have prognostic significance on outcome after ASCT, but its safety and efficacy remain uncertain for patients over that age. Nowadays, induction followed by autologous stem cell transplantation (ASCT) after high-dose melphalan conditioning continues the standard treatment for MM patients under the age of 65 years. Over the last two decades, there were significant advances in understanding MM disease biology and in development of several new drugs that allowed a paradigm shift from a palliative intent towards the active management of the disease aiming to prolong event-free survival (EFS) and overall survival (OS). A Mayo Clinic study confirmed a significant increase in cases diagnosed in older age groups when comparing to the 1950s and early 2000s, with the median age at diagnosis of MM increasing from 70 to 74 years, as well as doubling the proportion of newly diagnosed patients aged 80 years or older. On the one hand, the lengthening of life expectancy is related to an increase in the incidence of oncological diseases, and on the other hand, the improvement of diagnostic acuity and new therapeutic options on MM has led to a longer survival of elderly patients from median 19 months (in 1973) to 6.1 years (in 2004). Multiple myeloma (MM) is mainly a disease of the elderly. A higher dose of melphalan has more toxicity, but it is globally a well-tolerated procedure. Selected elderly patients when transplanted have similar disease response and survival as younger patients. Survival of transplanted elderly patients was superior to non-transplanted (OS, 59 months vs 30 months, p = 0.037 EFS, 45 months vs 27 months, p = 0.014). Non-transplanted elderly patients had comparable disease features, and induction response was similar in both groups (before ASCT in the transplanted cohort). Global transplant-related mortality was 3.8%. Those patients also had higher needs of transfusional support, higher grade of mucositis ( p = 0.028), and more days of intravenous antibiotics ( p = 0.019) than the elderly transplanted with MEL140. Stratifying by age, there were no statistically significant differences concerning transplant-related myelotoxicity and non-hematopoietic toxicity however, elderly patients conditioned with MEL200 had higher needs of transfusional support and more days of intravenous antibiotics. Conditioning consisted of melphalan 200 mg/m 2 (MEL200) in younger patients and melphalan 140 mg/m 2 (MEL140) in half of elderly patients. We analyzed a total of 155 patients, 132 of which underwent ASCT (≤ 65 years, n = 103, median 56 years > 65 years, n = 29, median 67 years) and 23 non-transplanted (median 68 years). A non-transplanted group with similar clinical characteristics, aged 65–70 years old, diagnosed and treated in the same timeline was used for comparison. We performed a retrospective analysis of newly diagnosed MM patients who underwent ASCT between January 2010 and July 2016. 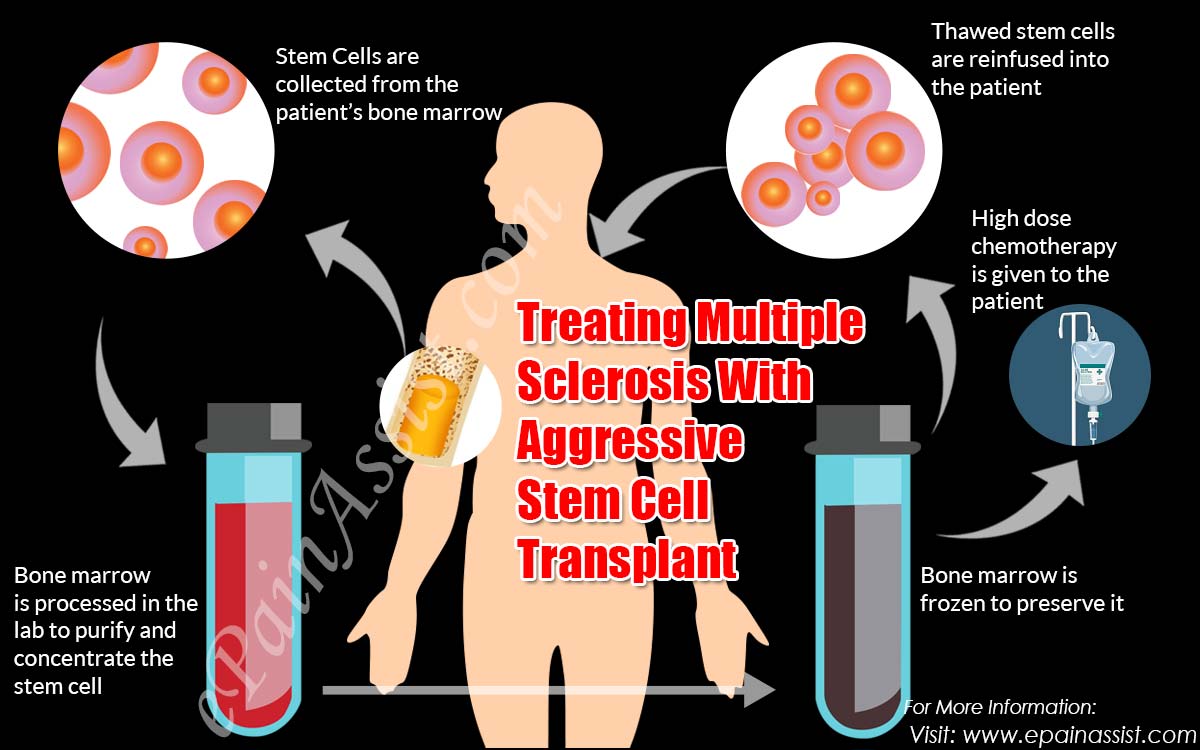
Autologous stem cell transplantation (ASCT) is still debatable in treatment of patients over 65 years with multiple myeloma (MM). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
